Cross-Linking FAQ: How Successful is iLink® FDA-Approved Cross-Linking?
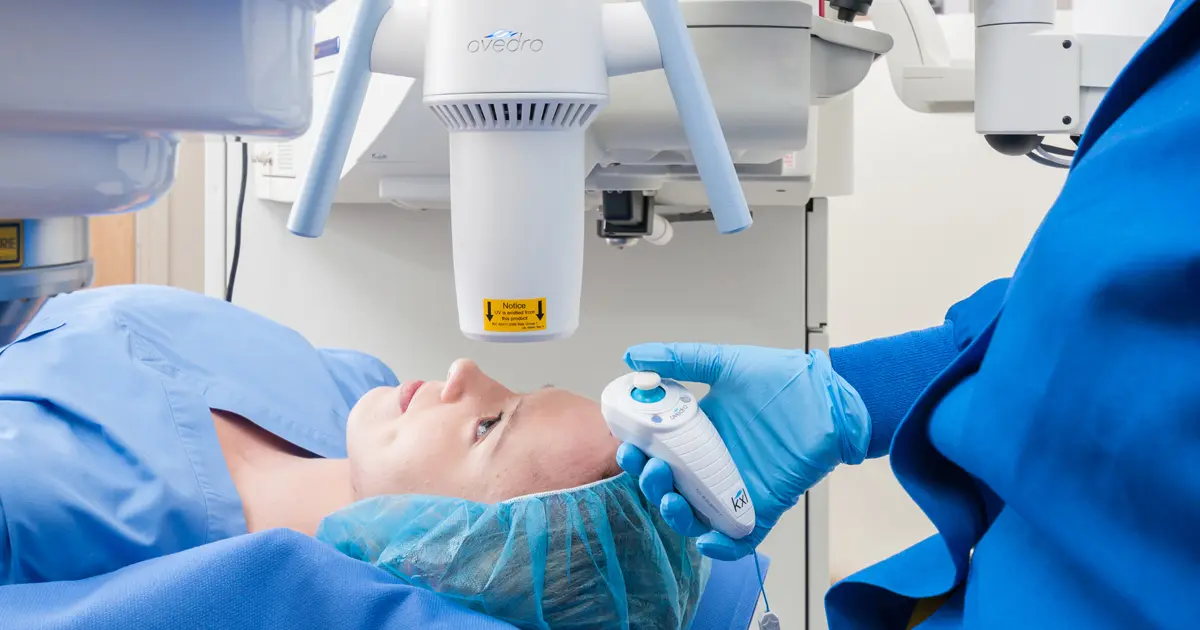
If you or a loved one has been diagnosed with progressive keratoconus, it’s likely that your physician has recommended or at least mentioned corneal cross-linking as a treatment option. iLink® FDA-approved cross-linking is a minimally invasive outpatient procedure intended to slow or halt the progression of keratoconus.
We know being diagnosed with a progressive condition can be daunting, and you likely have a lot of questions. With any treatment, one of your first thoughts might be “will the procedure work?” To help, we’re discussing the efficacy of FDA-approved cross-linking and sharing how some people in the Living with KC community are doing after receiving this procedure which preserves sight for many of the recipients.
How Successful is iLink® FDA-Approved Cross-Linking?
The goal of iLink® FDA-approved cross-linking is to stiffen the cornea to slow or prevent further progression of keratoconus and preserve vision. This epi-off cross-linking procedure with Photrexa® Viscous (riboflavin 5’-phosphate in 20% dextran ophthalmic solution), Photrexa® (riboflavin 5’-phosphate ophthalmic solution), and the KXL® system is the first and only cross-linking procedure shown to be safe and effective by the FDA and has been validated in clinical trials.
In the study that led to the FDA approval of iLink®, people who did not undergo cross-linking experienced progression of their condition, while those who underwent iLink® cross-linking did not.[1][2]
“We saw significant improvements in the steepness of the cornea and visual acuity, as well as subjective improvements across several measures of visual function, such as improved night driving.” – Peter Hersh, M.D., lead author, and corneal specialist at The Cornea and Laser Eye Institute
CLEI Center for Keratoconus
While the goal of the procedure is to slow progression to preserve vision, it’s important to note that cross-linking is not intended to eliminate or reduce dependence on refractive correction. Since iLink® is not intended to improve vision, but rather to halt the progression of the condition, many people will still need to wear corrective contact lenses or prescription eyeglasses following the procedure. Ideally, once progressive keratoconus is treated with iLink®, reduced changes in corneal curvature may make it easier to fit patients for contact lenses and many find their prescription does not change as frequently.
Over 400,000 iLink® cross-linking procedures have been performed worldwide with Glaukos’ equipment[1]. Both the American Academy of Ophthalmology and the Cornea Society recommend cross-linking for the treatment of progressive keratoconus.[2][3] Specifically, iLink® FDA-approved cross-linking is:
- Proven Safe & Effective: iLink® cross-linking is a minimally-invasive treatment proven by the FDA to be safe and effective in slowing or halting the progression of keratoconus to preserve vision.
- FDA-Approved: iLink® is the first and only FDA-approved corneal cross-linking procedure and has been approved in the United States since April 2016.
- Validated in Clinical Trials: Following two successful Phase III trials, iLink® received approval in 2016[4]. In clinical studies, cross-linking–treated eyes showed increasing improvement in Kmax from month 3 through month 12, while in untreated, sham eyes,[1] Kmax demonstrated steepening. Unlike iLink®, unapproved drugs and devices have not been validated and their manufacturing process has not been evaluated.
- Widely Covered by Insurance: iLink® cross-linking is widely covered by insurance and is the ONLY cross-linking procedure eligible for reimbursement in the U.S. Greater than 95% of the commercially insured population has access to this potentially sight-protecting treatment. Insurance does not typically cover products and procedures that have not received FDA approval or have not been proven to be safe and effective through clinical trials. A doctor should not ask you to pay cash and submit to insurance on your own.
“Now that cross-linking is available clinically, FDA approved, it is a very exciting time to be a cornea specialist and be able to have a treatment that is effective for progressive keratoconus.”
Dr. Kathryn Hatch, Massachusetts Eye and Ear Institute
| Category | iLink®: the ONLY cross-linking procedure approved by the FDA | Non FDA-Approved procedures |
|---|---|---|
| Drugs Used | Rigorously tested and controlled FDA-approved Photrexa®, Photrexa® Viscous | Riboflavin that has not been FDA-approved |
| Device Used | KXL® system, the only FDA-approved cross-linking device | Unapproved device used may have been modified or illegally imported, no post-market surveillance |
| Procedure | Epi-off procedure, validated in controlled clinical trials | Not FDA-approved: No standardized treatment approach |
| FDA Approved | Yes, for both Photrexa drug formulations and device used | No |
| Pivotal Clinical Trials | Yes, robustly studied procedure | No |
| # of US Procedures Performed | More than 60K | Unknown/Illegal |
| # of US physician performing procedure | 600+ | Unknown/Illegal |
| Adverse event reporting | FDA-mandated reporting & approved labeling with known risks/side effects (see prescribing information) | Side effects not tracked or monitored |
| Insurance Coverage | >95% commercial coverage; All 50 states have >6 plans covering iLink® | No; fully out of pocket cash procedure |
With any medical procedure, there are potential side effects. Common ocular side effects include haze, inflammation, fine white lines, dry eye, disruption of surface cells, eye pain, light sensitivity, reduced sharpness of vision, and blurred vision. The iLink® procedure is not right for everyone so talk to your physician to discuss what treatment option is right for you.
What Do People in the Living with KC Community Have to Say?
iLink® cross-linking is a safe and effective FDA-approved treatment option to slow or halt the progression of keratoconus. But don’t just take our word for it – members of the Living with Keratoconus community* have received iLink® and shared their experiences from diagnosis to treatment and beyond.

Casey: At just 15 years old, Casey started experiencing blurry vision and had to get creative to manage everyday activities. With his vision issues under control after receiving iLink® FDA-approved cross-linking, Casey is thrilled to have his life back on track. He’s looking forward to pursuing many of his dreams without his vision getting in the way. He recommends the FDA-approved cross-linking procedure to anyone who is struggling with progressive keratoconus, and he now lives by the motto, “Why waste time adapting to life when you don’t have to?”

Chris: Now that his keratoconus has been treated, Chris believes that he has been given a second chance to excel at his career. He encourages others to get their eyes checked regularly and to keep asking questions if their doctors are unable to identify a diagnosis. “Baseball has been a part of my DNA since I could pick up a bat. This surgery…has given me kind of a second chance at being able to do things at a level I never thought I would be able to do.”
Remember, you’re not alone in your journey! To learn more about people who have undergone iLink® FDA-approved cross-linking, read their Keratoconus Journeys today.
*Results may vary.
Don’t Wait to Schedule Your Appointment!
We hope you found this information on iLink® cross-linking helpful and were inspired by the stories from the Living with KC community. For many, FDA-approved cross-linking has helped to slow or halt the progression of their keratoconus, and their vision has been improved with the use of contact lenses! [5]
“We report good visual results in patients who were fit in contact lenses after having undergone corneal cross-linking. Contact lens fits were as early as two weeks (soft lenses), but ranged depending on patient’s functioning needs and observed changes in corneal topography in the postoperative healing period. Gas permeable lenses were fit at the earliest 3 months postoperatively. Contact lens choice is a balance between patient’s needs and the lens able to achieve good comfort with optimal visual results.”
Clark Chang, OD, MS
For more information on cross-linking, read our Cross-Linking FAQ blog series. If you’re looking for a physician in your area that is offering this FDA-approved treatment, visit our website. You can also follow us on Facebook, Twitter, and Instagram!
Resources
[1] Data on File, Glaukos, Inc.
[2] Belin MW, Lim L, Rajpal RK, et al. Corneal cross-linking. Cornea. 2018;37(10):1218-1225.
[3] Garcia-Ferrer FJ, Akpek EK, Amescua G, et al. 2018 American Academy of Ophthalmology: Corneal Ectasia Preferred Practice Patterns: Ophthamol 2018;126(1)170-215
[4] Photrexa [package insert]. Waltham, MA: Glaukos, Inc. 2016.
[5] Kreps, E. O., Pesudovs, K., Claerhout, I., & Koppen, C. (2021). Mini-Scleral Lenses Improve Vision-Related Quality of Life in Keratoconus. Cornea, 40(7), 859–864.