What To Know About Corneal Topography – Part 2
Now that we’ve talked about how keratoconus is diagnosed and what corneal topography is, it’s time to focus on what to expect during the testing process. Any type of eye test or procedure can be a potentially stressful experience, so it’s important to learn the facts before going into the doctor’s office.
In Part 2 of our topography blog series (go back to Part 1), we’re discussing the corneal topography testing experience and how your results will ultimately be used to determine a keratoconus diagnosis.
What should I expect when getting corneal topography?
How long will it take to complete?
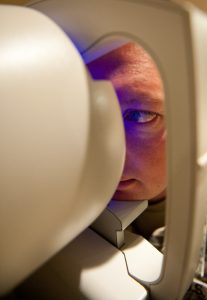
Getting corneal topography is a lot like having a picture taken of your eye. Typically, you will sit in a chair and place your chin on a chin rest. You will be asked to look at a light or other target in the bowl of the topography camera. Then, you will be asked to keep your eye open for a few seconds while an image is obtained.
There is no puff of air or other contact with your eye during the topography measurement. After the image is obtained, you’ll be allowed to blink normally while the topography computer uses the images captured to generate a map of corneal curvature.
The process may need to be repeated a few times before a high-quality image is obtained. Often, your doctor will review this map with you on the day of the exam, or you may review with your doctor during a future visit.
Will I feel any discomfort during or following corneal topography?
Corneal topography is a painless, non-contact technique, meaning that the corneal topography device will not touch your eye during the measurement. If your eye is dry you may have a few moistening drops instilled into your eye to improve the quality of the topography image.
How will the results be used to guide my treatment?
Corneal topography provides your doctor with detailed information about the shape of your eye. If you have keratoconus, topography allows your doctor to determine whether it is mild, moderate or severe, and repeat measurements provide information about whether your keratoconus is progressing. This information is useful in determining the best options for visual correction and can be used to guide contact lens fitting.
Learn more: What You Need To Know About Corneal Topography – Part 1
To find a doctor near you to get screened for keratoconus, use our locator tool.