Talking to Your Doctor
This valuable discussion guide may help you talk to your doctor about KC, the screening process, and your treatment options
What to expect during an evaluation
Your doctor will provide a comprehensive eye exam for keratoconus that may include diagnostic tools, such as a corneal topographer, corneal tomographer, and a corneal pachymetry test:
The corneal topographer
will take a picture of the surface of your eye to detect potential subtle changes of the surface of the eye.
The doctor may also use a corneal tomographer, which looks similar.
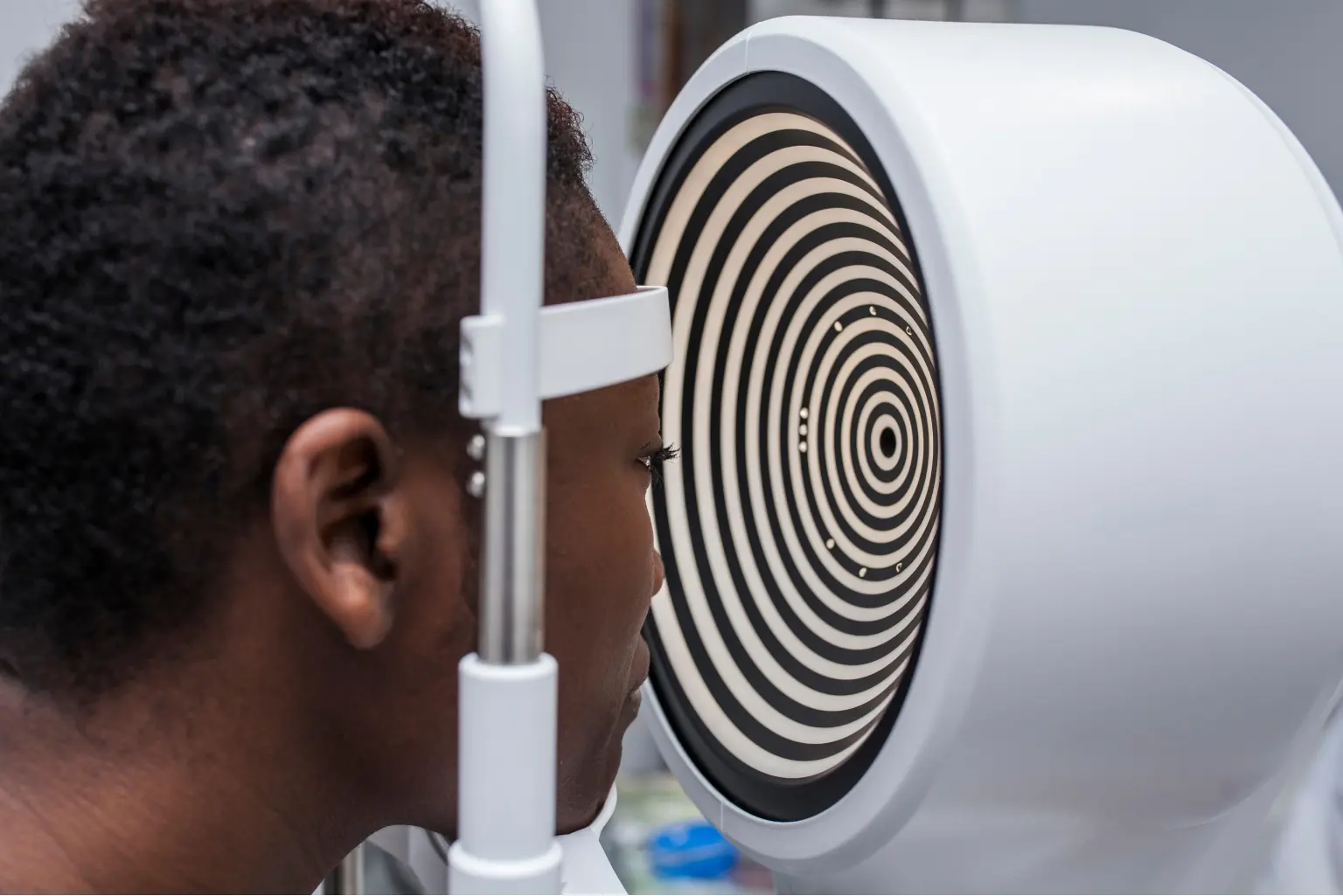
The corneal tomographer
is an instrument that measures the thickness of the cornea at different locations, especially on the back surface of the cornea. It can be especially valuable because it could detect KC before the cornea starts to form a cone shape.
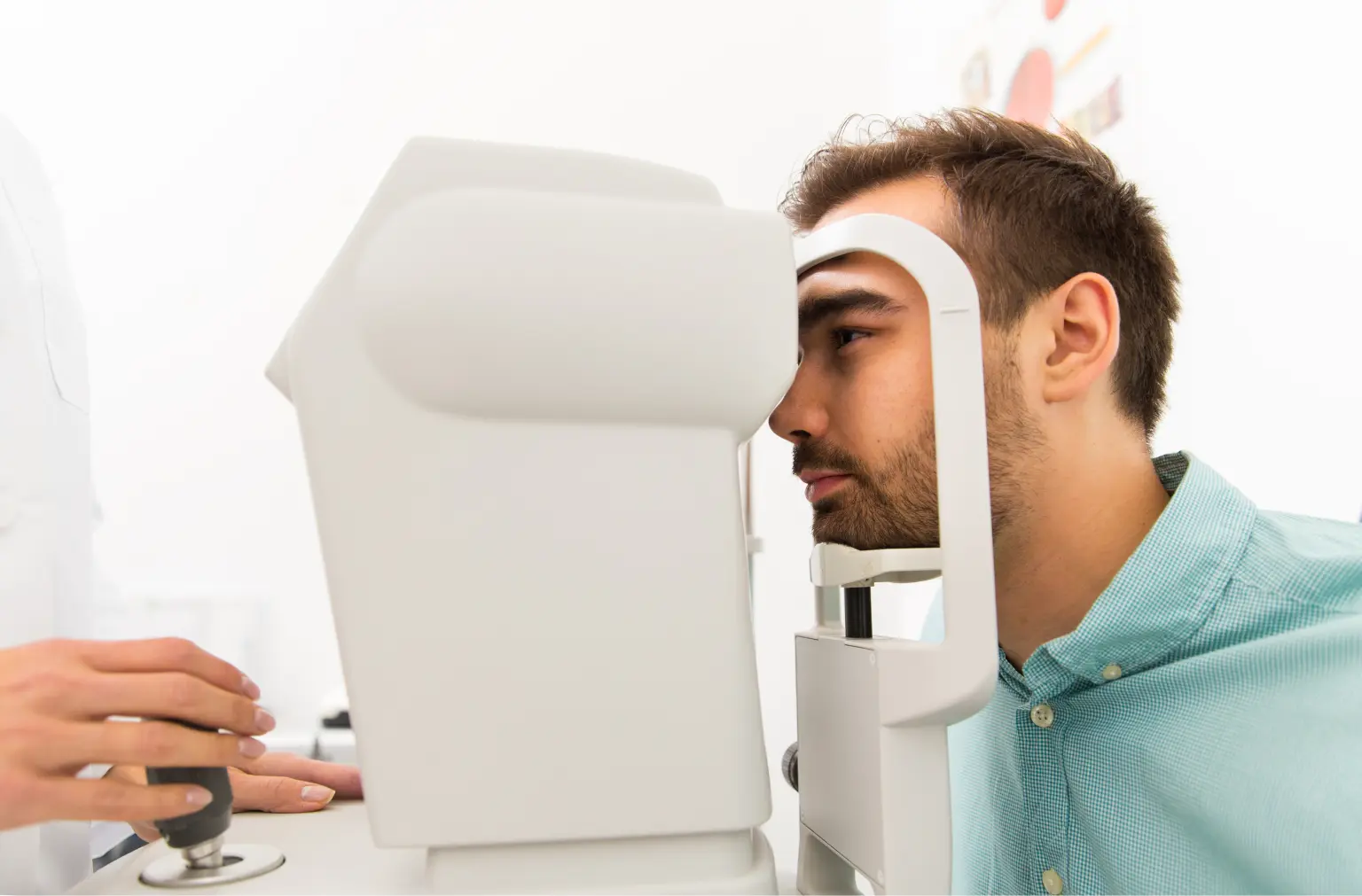
Corneal pachymetry
is a third possible test which measures the thickness of the cornea to show progressive thinning over time.
