Blogs
-

Taking the Plunge: Shradha’s Journey to the Depths of the Ocean with Keratoconus
Read more: Taking the Plunge: Shradha’s Journey to the Depths of the Ocean with KeratoconusBy: Shradha I was diagnosed with keratoconus at a time in my life when I was enthusiastic about changing the world. What I ended up changing, however, were seven prescriptions and five doctors over the course of two years, before a specialist finally diagnosed my condition. These were not the only changes I was dealing […]
-
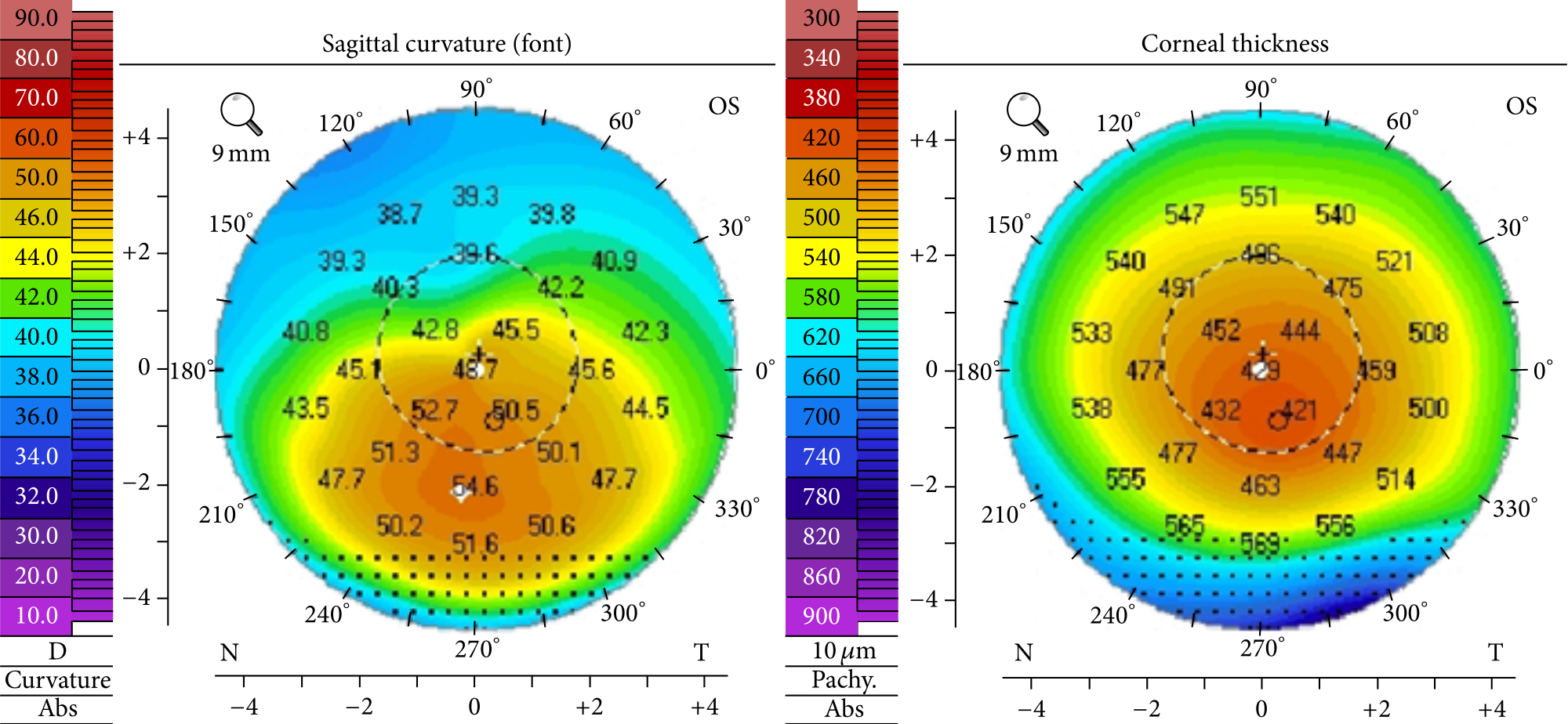
Corneal Topography – What to Know & Why It’s Important – Part 1
Read more: Corneal Topography – What to Know & Why It’s Important – Part 1Whether you’ve worn glasses or contacts for years or not, realizing your vision is declining can be a scary experience. For patients suspected to have keratoconus, doctors may order multiple tests with corneal topography.
-

Corneal Topography – What to Expect in the Exam – Part 2
Read more: Corneal Topography – What to Expect in the Exam – Part 2Now that we’ve talked about how keratoconus is diagnosed and what corneal topography is, it’s time to focus on what to expect during the testing process.
-

Your Child Has Been Diagnosed with Keratoconus…Now What?
Read more: Your Child Has Been Diagnosed with Keratoconus…Now What?As a parent, you always want what’s best for your child and you want them to be healthy. While any medical news or diagnosis may come as a shock, oftentimes there are options available to treat or manage the condition.
-

Tips for Coping With a Keratoconus Diagnosis
Read more: Tips for Coping With a Keratoconus DiagnosisIf you or a loved one has recently been diagnosed with keratoconus, you may be feeling all sorts of emotions – confusion, worry, fear, anxiety, or maybe all of the above. At Living with KC, we want to offer some advice and provide strategies to help you manage your emotions.
-

Tips for Coping with Headaches and Light Sensitivity
Read more: Tips for Coping with Headaches and Light SensitivityHeadaches and light sensitivity are two common conditions that you most likely have heard of before or experienced firsthand. Although there are some easy fixes for these uncomfortable and sometimes inconvenient conditions, it can be stressful if they continue to occur without a known or obvious explanation.
-

A Seasonal Guide to Allergies
Read more: A Seasonal Guide to AllergiesDo you feel like you’re affected by allergies year-round? You’re not alone! Hay fever affects about 6.1 million children and 20 million adults. While many people associate allergy season with the fall or spring, few know there are different allergens that can make your symptoms flare-up year-round.
-

Feel Confident Taking the Wheel at Night
Read more: Feel Confident Taking the Wheel at NightDo you consider yourself a good driver? Most of us should feel confident behind the wheel, but do you ever feel that your driving ability changes when the sun goes down?
-

Down Syndrome & Keratoconus – What You Need to Know
Read more: Down Syndrome & Keratoconus – What You Need to KnowDown syndrome can affect the maturing eye which can impact the proper development of vision in children and adults. More than half of people with Down syndrome experience an eye disease at some point in their lives, so caregivers and doctors should monitor their vision closely.
-

Dr. Audrey Talley-Rostov on Increasing Awareness for Keratoconus
Read more: Dr. Audrey Talley-Rostov on Increasing Awareness for KeratoconusWhile symptoms for keratoconus often first appear in the late teens and early twenties, there are instances where a diagnosis may come later in life. Keratoconus can often be misdiagnosed…
-

The Emotional Impact of a Keratoconus Diagnosis
Read more: The Emotional Impact of a Keratoconus DiagnosisScared, worried, and confused are just a few of the emotions that people use when describing how they felt after a keratoconus diagnosis. Long-term illnesses can have a big impact on the daily lives of patients…
-

Keratoconus in the Workplace: What You Need to Know
Read more: Keratoconus in the Workplace: What You Need to KnowResearch shows that signs of keratoconus primarily appear in the late teens and early twenties, meaning that for many patients, a diagnosis may occur when they are beginning to plan their futures after high school and college.
-

Is Keratoconus Hereditary? A Mother’s Perspective
Read more: Is Keratoconus Hereditary? A Mother’s PerspectiveAs a mother of three boys, one of my biggest concerns is their health. Throughout your children’s lives you try to give them the resources they need to be successful – whether that’s playing sports, excelling in the classroom, taking up a musical instrument or acting in the school play.
-

Infographic: Understanding Keratoconus & the Importance of Early Diagnosis
Read more: Infographic: Understanding Keratoconus & the Importance of Early DiagnosisFor those living with the disease, understanding keratoconus can be difficult, especially the complexity of the condition and how it can affect your eyesight.
